
Diplomate American Board of Orofacial Pain
9615 Brighton Way, Suite 323
Beverly Hills, CA 90210
888.981.8981
Radiology for the TMJ
Radiology is needed to see what is occurring with the hard tissues of the TMJ, which stands for temporomandibular joint, and is occasionally needed for the soft tissues of the TMJ. At my Beverly Hills TMJ practice, if I need imaging of the TMJ, I will usually want to see what the hard tissue looks like, which means obtained a cone beam computed tomography, or what is abbreviated at CBCT or cone beam CT. This enables the radiologist and me to see a 3D image of your jaw and then those images can be sliced so we can obtain single images such as those that you see below. An MRI is needed if we need to see the soft tissues but in most cases, MRI's are not needed.
What is interesting about this case is that the images are from the same patient. She was 39 years old when I saw her for the first time. She reported being knocked unconscious by a basketball to the left side of her face when she was 12 years old. She received physical therapy after the incident but years later developed pain in the joint. She was treated with a nighttime only appliance, given some muscle stretching exercises and a hinge-axis exercise to help stimulate synovial fluid, and some anti-inflammatories. After a couple of months, her range of motion improved and the pain resolved.
Normal Imaging of the TMJ
 |
 |
 |
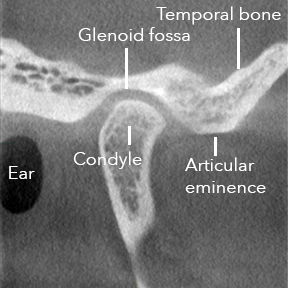
| This is a normal appearing image of the right TMJ. You are looking at a section of the head through the jaw from the side. |
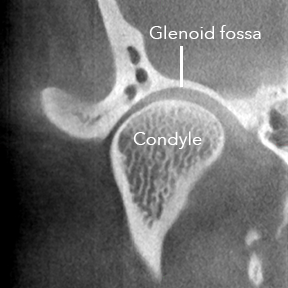
This is a normal appearing image of the right TMJ. You are looking at a section of the head through the jaw from the front to the back. |
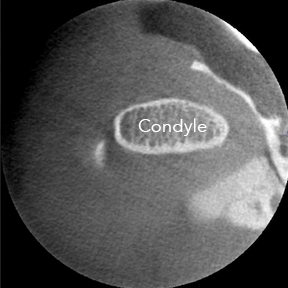
This is a normal appearing image of the right TMJ. You are looking at a section of the head through the jaw from the top looking down. |
What makes the above series of images normal are all of the following:
- There is a thin white line around the perimeter of the condyle. We call this
cortication , and it tells us the outside layer of the bone is nice and dense. Inside the condyle, there is a spongy appearance, which we call trabeculation, and it tells us the inside layers of the bone are very light. The surface of the condyle is smooth. - The Glenoid fossa is smooth and shaped like a horseshoe.
- There is about an equal amount of space between the condyle and the Glenoid fossa. This space is occupied by the disc that is a cushion between the bone of the condyle and the temporal bone.
Abnormal Imaging of the TMJ - Osteoarthritis
 |
 |
 |
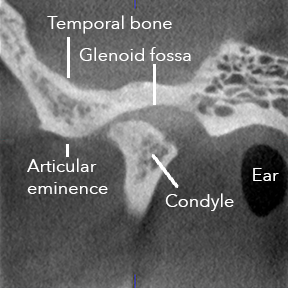
| This is an abnormal appearing image of the left TMJ. You are looking at a section of the head through the jaw from the side. |
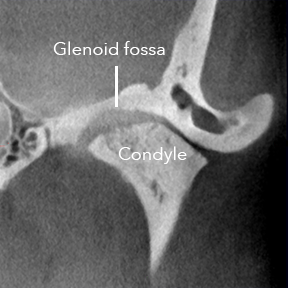
This is an abnormal appearing image of the left TMJ. You are looking at a section of the head through the jaw from the front to the back. |
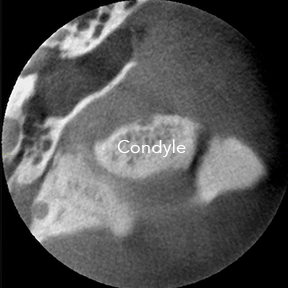
This is an abnormal appearing image of the left TMJ. You are looking at a section of the head through the jaw from the top looking down. |
What makes the above series of images abnormal are all of the following:
- There is a very thick white area around the perimeter of the condyle, which means the bone is very dense and heavy. Inside the condyle, there is almost no spongy appearance, and it tells us the inside layers of the bone are heavy. The surface of the condyle is rough and irregular.
- The Glenoid fossa is not shaped like a
horseshoe, and is not as smooth as the normal images in the top series of pictures. - There is
an unequal amount of space between the condyle and the Glenoid fossa. This tells us that the disc is likely displaced forward of where it should be.
The images above are an example of severe osteoarthritis. This joint is likely to make a grinding/grating "rice
Learn about TMJ movement and range of motion.
Learn about the muscle referral patterns of the jaw closing muscles.
Learn about the muscle referral patterns of the muscles that refer pain into the TMJ.






