
Diplomate American Board of Orofacial Pain
9615 Brighton Way, Suite 323
Beverly Hills, CA 90210
888.981.8981
More About TMJ
TMJ Animations and Range of Motion
The temporomandibular joint is a very unique joint. It is the only joint in the body that requires two joints to be moved and it is the only joint in the body that has two movements. A normal joint does not click. A clicking joint without pain does not necessarily need treatment other than a hard full coverage nighttime appliance. Some patients need a top and bottom, which can reduce the clicking. If you click when you open, the medical term is anterior disc displacement with reduction. If you used to click when you opened but you no longer do and your opening is very limited compared to when it was clicking, you most likely have a "closed lock," meaning you cannot open very wide. The medical term is anterior disc displacement without reduction, and the jaw cannot get onto the disc. If you are stuck open, you have an "open lock," which is usually very easy to treat. The medical term for this is a dislocation or subluxation.
It is important to determine if a limited range of motion is due to a mechanical issue with the disc or an issue of tight muscles. Knowing the range of motion is a key factor.

TMJ Range of Motion Measurements
A patient’s range of motion measurements should be recorded as part of every new patient exam. This adds about 10 seconds to a new patient exam if you only record the three opening movements, which are “comfort, active, and passive.” If you measure right and left lateral and protrusive movements, you might be adding 60 seconds to your exam time. Yes, it’s that quick.
Normal Range of Motion
Opening: 40 to 60 mm. If a patient opens to 55 mm with either the comfort or active opening, there is no need to obtain the Passive opening. Additionally, do not have a patient open past 60 mm and do not push a patient open past 60 mm. If they can open to 60 mm or you can push them to 60 mm, then they have an excellent opening range of motion.
Lateral: 8 to 12 mm
Protrusive: 8 to 12 mm
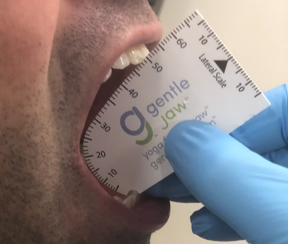
Opening Movements
Place the notch of the range of motion scale on the midline of the mandibular centrals, and take the following three measurements:
Comfort: ask the patient to open “comfortably without pain.”
Active: ask the patient to open as wide as they can even if it hurts.
Passive: with the patient in the Active opening, the doctor then pushes the patient open using their thumb on the maxillary centrals and their index or middle finger on the mandibular centrals. This might hurt the patients but this measurement is key. If you are pushing hard, and the patient is fighting you but you can push more, we call this a "soft end feel." If you are pushing hard, and it feels like you are pushing down on a granite countertop, we call this a "hard end feel." If you record a hard end feel of about 30 mm or less, then it is likely a closed lock, and the issue is the articular disc of the TMJ is inflamed and it is preventing the condyle from getting onto the disc. If a patient can open past 30 mm and it is a soft end feel, then it is likely a muscular issue, and passive jaw stretching with the gentle jaw will help increase the range of motion.
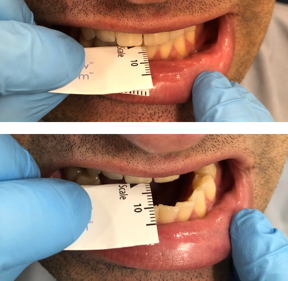
Protrusive Movement
Fold the range of motion scale in half at the black triangle on the lateral scale. Measure the overjet, then ask the patient to move their jaw forward “like a bulldog” and measure that number. Record those two numbers as separate numbers such as “2+8” so that you know the overjet plus how far they can protrude forward from their centric occlusion.Note in your chart if any of the movements cause pain and if any of the movements replicate their jaw pain. If a movement does cause pain, have the patient point with one finger where the pain occurs
If the patient ever has a future problem with opening and/or moving their jaw, you now have a baseline of what their normal movements are. Do you think it is worth spending up to one additional minute of your time to record these measurements? You will if you ever have a patient who has a problem especially if they think you created it with an injection or by keeping them open too long.
Lateral Movements
With the arrow of the range of motion scale centered on the maxillary centrals, have the patient move to the left by tapping the mandible on the left, which causes the patient to move to the side that you are 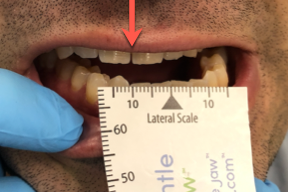 tapping. Measure the distance traveled. Repeat this for the right side by tapping the right side of the jaw.
tapping. Measure the distance traveled. Repeat this for the right side by tapping the right side of the jaw.
As always, I’m happy to help any patient who is experiencing jaw pain or any facial pain including migraines, trigeminal neuralgia, sleep apnea or snoring issues at my office in Beverly Hills. Please let me know how I can help or if you have any questions.
TMJ Animations
A normal TMJ disc does not click when the jaw is opened and closed, and when it is moved side to side. A TMJ disc that does click usually does not cause pain. Please view the animations below and read the text below the animation to learn more.
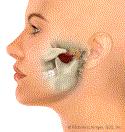 Normal Functioning Jaw
Normal Functioning Jaw
Normal opening: The disc, which is shown in yellow, is in the proper position and it glides forward and back when the jaw is opened. The above animation was developed by a medical illustrator under the guidance of Dr. Hirschinger.
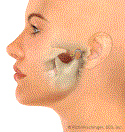 Popping Jaw
Popping Jaw
Popping or clicking jaw: The disc, which is shown in yellow, is forward, or anterior, of the jaw condyle. When the jaw is opened, the disc can click or pop, and then the jaw follows its normal opening. Clicking can also occur on closing. When this occurs, it is known as anterior disc displacement with reduction. The above animation was developed by a medical illustrator under the guidance of Dr. Hirschinger.
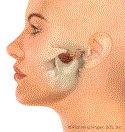 Closed Lock
Closed Lock
Closed lock: The disc is forward of its normal position and it prevents the jaw from fully opening. This is called a closed lock or anterior displacement without reduction. The above animation was developed by a medical illustrator under the guidance of Dr. Hirschinger.
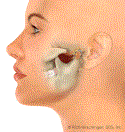 Jaw Dislocation
Jaw Dislocation
Subluxation or dislocation. If the jaw opens too wide, it can get stuck in the wide open position, which is called an open lock. A patient can rarely get the jaw closed, which is why you should call us if this happens to you. The above animation was developed by a medical illustrator under the guidance of Dr. Hirschinger.
Learn about the muscle referral patterns of the jaw closing muscles.
Learn about the muscle referral patterns of the muscles that refer pain into the TMJ.
Learn about TMJ CBCT radiology.






